
In order to accomplish its objective of “affordable health insurance coverage”, the Affordable Care Act (ACA) created three (3) separate, cost reducing initiatives: 1. Premium Tax Credits – reduce out of pocket PREMIUM costs; 2. Cost Sharing Reductions (CSR) – reduce point of service out of pocket costs such as copays, deductibles, and coinsurance; andLEARN MORE

This particular blog post is primarily directed to residents of my adopted home state of Nebraska. However it may shed light on some of the “when’s, who’s and what’s” that health care/insurance stakeholders may be facing in other parts of the country next year. As we inch closer to the 2018 individual health insurance openLEARN MORE

On May 4, 2017, the U.S. House of Representatives passed an amended version of the “American Health Care Act” or AHCA, on a 217-213 vote tally. In and of itself, this vote DOES NOT ALTER THE HEALTHCARE/HEALTH INSURANCE LANDSCAPE! There are a number of phases (at least 3, but likely several more procedural steps) that must be completed in order for the Affordable Care Act (ACA) to be partially repealed. And to be clear, the AHCA would represent a partial, piecemeal repeal of the ACA, and would in fact, retain much of the ACA. So here’s where we are and what we know, as of today…

Patient Centered Outcomes Research Institute (PCORI) Fee, also known as the Comparative Effectiveness Research Fee (CERF)Fee periods and payment schedule For CERF payments, ERISA plan year is important, and determines both the timing and amount of payment to the IRS. If your ERISA plan year and renewal date differ, the ERISA plan year should be usedLEARN MORE
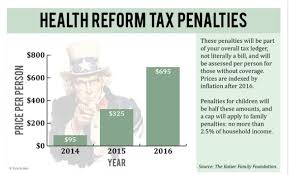
The Affordable Care Act’s (ACA) “health insurance mandates” are still in effect, and have most definitely not been abolished. Had the Republican party’s – The American Health Care Act (AHCA) – passed, it would have, among other things, retroactively eliminated both the Individual and Employer mandates. As such, it did not go to aLEARN MORE

Until recently (late February, 2017), talk of “repealing/reforming/replacing” the Affordable Care Act (ACA), aka Obamacare, has been largely speculative. We now have our first look at draft legislation that aims to replace major aspects of the ACA. It is important to note that what is being considered is not a wholesale repeal of the ACA,LEARN MORE

Last Friday (11/18/2016) the IRS announced extended deadlines for the delivery of forms 1095-B & C to INDIVIDUALS. IRS forms 1095-B and 1095-C must now be provided to affected individuals no later than March 2, 2017 (originally 1/31/2017). Please note this extension does NOT apply to the deadlines for filing forms 1095-C, along with 1094-C, 1094-B, andLEARN MORE
By one count (The Galen Institute); there have been seventy (70) significant changes, delays, modifications, and partial repeals of the Affordable Care Act (ACA)/Obamacare to date. (For those keeping score at home, 43 have come from the White House; 24 from Congress; and 3 from the Supreme Court.) The challenges for stakeholders lie not only in developing sound, effective compliance strategies, but in keeping up with the various fits and starts of the law. In addition, various penalties, fees, taxes, limits, and safe harbors are indexed for inflation, and thus, subject to change on an annual basis. Listed below are some of the more relevant and timely announcements which impact ACA compliance in 2016 and beyond:
Yesterday (October 7, 2015) the President signed the Protecting Affordable Coverage for Employees, or PACE Act, giving states the flexibility to define “small employer group”, for purposes of the Affordable Care Act (ACA). The PACE Act also redefines the definition of small employer to 1 – 50 employees. This is an extremely important tweak toLEARN MORE
Yesterday (October 7, 2015) the President signed the Protecting Affordable Coverage for Employees, or PACE Act, giving states the flexibility to define “small employer group”, for purposes of the Affordable Care Act (ACA). The PACE Act also redefines the definition of small employer to 1 – 50 employees. This is an extremely important tweak to the ACA, especially for employer groups that employ between 50 – 100 full and part-time employees.